Food allergy symptoms
The symptoms of food allergy range from mild discomfort to a severe, life-threatening reaction called anaphylaxis, which requires immediate medical treatment.
The most frequent symptoms of food allergies are itching or swelling of the mouth. Other symptoms include sneezing, blocked nose, a rash or hives, and stomach upset.
Symptoms usually begin within the first 5-30 minutes of exposure, but may occur up to several hours later (Rutkowski, Dua and Nasser, 2012).
The symptoms arise every time the allergic person eats the offending food. However, if they are allergic to a food that is cross-reacting with pollen they may only experience symptoms in the pollen season.
Different kinds of food poisoning can provoke symptoms that are similar to the symptoms experienced in food allergy. In order to distinguish between a food allergy and food poisoning the person with symptoms needs to see a doctor.
Allergic reactions to foods may occur within a few minutes after eating the food, but rarely symptoms may also develop after hours, making the relationship with ingestion of food less clear.
Symptoms generally disappear within hours but can last for days. The specific symptoms and severity of an allergic reaction are affected by:
- the type and amount of the allergen consumed;
- the form in which the food containing the allergen was eaten;
- the intake of alcohol, aspirin and other drugs such as beta-blockers and ACE inhibitors;
- exercise;
- stress;
- the sensitivity of the allergic person.
The symptoms may appear in different parts of the body:
Mouth
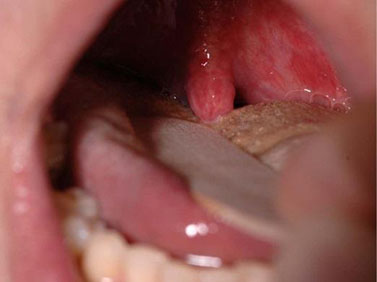 The most frequent symptoms of food allergies are itching and/or swelling of the mouth.
The most frequent symptoms of food allergies are itching and/or swelling of the mouth.
Oral itching (known as oral allergy syndrome) can be an initial symptom in any kind of food allergy.
However, oral itching is a well-known symptom in food allergy induced by cross-reaction with pollen. It can happen with foods like apple, kiwi, hazelnuts, walnuts, celery, carrot, tomato, cherry, and melon.
Most of the allergens involved in pollen-related cross-reacting foods will be destroyed in the gastrointestinal tract. This explains why the symptoms are frequently mild and limited to the mouth.
Most of the allergens in the cross-reactive foods will also be destroyed if the food is cooked. This explains, for example, why many birch pollen allergic people cannot eat raw apples without experiencing symptoms but stewed apples and apple juice might not be a problem.
Eyes and nose
The eyes and nose may show hay fever-like symptoms. The eyes may swell, itch, and become red.
Sneezing and an itchy and runny (or stuffed) nose may be experienced.
Lungs
Asthmatic symptoms such as wheezing, breathlessness and coughing may arise from the lungs.
Stomach
Symptoms from the stomach include pain, bloating, nausea, vomiting, and diarrhoea.
Skin
On the skin, an acute nettle rash (also called urticaria or hives) with itchy, well-defined white or pale red swellings can appear.
This rash is generally short-lived, disappearing within hours. Chronic nettle rash is rarely associated with food allergy.
Longer lasting, chronic skin reactions in the form of atopic dermatitis are associated with food allergy, especially in children.
Anaphylaxis
Anaphylaxis is an uncommon, acute, potentially life-threatening and sometimes fatal allergic reaction involving the whole body.
The skin itches, the affected person becomes unwell and dizzy, they feel their heart beating, they feel nauseous, and everything may go black. At the same time they may get nettle rash, hay fever, and suffer an asthma attack. Their blood pressure may drop, and they may faint. Untreated anaphylaxis can rapidly result in death.
In Europe and the US, peanut and tree nuts are the foods most commonly reported to cause anaphylaxis. Prompt administration of adrenaline after eating suspected problem foods and transport to an emergency department has helped minimise life-threatening episodes.
Food allergies are one of the most common causes of anaphylaxis and account for approximately 30% of all fatal cases of anaphylaxis (Lieberman et al. 2010). Within in the United States, peanut induced anaphylaxis alone, affects 1.5 million people and leads to between 50-100 deaths each year (Wen et al. 2007).
Anaphylaxis can be persistent and reoccurring up to 8-12 hours after an initial attack (reoccurrence occurs in approximately 20% of cases). These effects cannot be predicted from the severity of the initial phase of anaphylaxis (Kemp and Lockey, 2002).
According to the Network for Online Registration of Anaphylaxis database, individuals with pre-existing cardiovascular conditions are associated with the most severe allergic reactions.
Further reading
- Sicherer, S. H. (2017) Food allergies: A complete guide for eating when your life depends on it
- Fu, L., Cherayil, B. J., Shi, H., Wang, Y., & Zhu, Y. (2019) Risk Assessment and Control Management of Food Allergens
- Rutkowski K, Dua S, Nasser S (2012) Anaphylaxis: current state of knowledge for the modern physician
- Lieberman, P., et al (2010) The diagnosis and management of anaphylaxis practice parameter: 2010 Update
- Wen, H. , Borejsza‐Wysocki, W. , DeCory, T. R. and Durst, R. A. (2007) Peanut Allergy, Peanut Allergens, and Methods for the Detection of Peanut Contamination in Food Products
- Kemp, S.F. and Lockey, R.F. (2002) Anaphylaxis: A review of causes and mechanisms
- Brockow K, Kneissl D, Valentini L, Turner PJ, Gowland MH, Sharma V, Ierodiakonou D, Harper N, Garcez T, Pumphrey R, Boyle RJ. (2015) Increase in anaphylaxis-related hospitalizations but no increase in fatalities: an analysis of United Kingdom national anaphylaxis data, 1992-2012
- Worm M, Moneret-Vautrin A, Scherer K, Lang R, Fernandez-Rivas M, Cardona V, Kowalski ML, Jutel M, Poziomkowska-Gesicka I, Papadopoulos NG, et al. (2014) First European data from the network of severe allergic reactions (NORA)
- Muraro A, Werfel T, Hoffmann-Sommergruber K, Roberts G, Beyer K, Bindslev-Jensen C, Cardona V, Dubois A, duToit G, Eigenmann P, Fernandez Rivas M, Halken S, Hickstein L., et al. (2014) EAACI Food Allergy and Anaphylaxis Guidelines Group. EAACI food allergy and anaphylaxis guidelines: diagnosis and management of food allergy
