
Annual report 2022: UK patient and general population data 2009-2019, and real-time surveillance data
Date of publication: April 2022
Our 2022 annual report provides findings relating to people who died by suicide between 2009 and 2019 across all UK countries. Additional findings are presented on the number of people under mental health care who have been convicted of homicide, and those in the general population.
Our large and internationally unique database is a national case series of suicide by patients under the care of mental health services over more than 20 years. This allows us to make recommendations for clinical practice and policy that will improve safety locally, nationally, and internationally.
In this year’s report, though we present data from deaths occurring between 2009 and 2019, most of the themed findings relate to groups that we now know are likely to have been particularly vulnerable during the COVID-19 pandemic: patients with economic difficulties, those who have been victims of domestic violence, and those with comorbid physical illness.
Key messages
Clinical risk
 Our findings show established risk factors for suicide – such as previous self-harm, alcohol or drug misuse, multiple mental health diagnoses, living alone – are common among patients who die by suicide. 1 in 10 patients were known to have died on or near an anniversary or significant date.
Our findings show established risk factors for suicide – such as previous self-harm, alcohol or drug misuse, multiple mental health diagnoses, living alone – are common among patients who die by suicide. 1 in 10 patients were known to have died on or near an anniversary or significant date.
We suggest clinicians assessing risk enquire about significant dates and anniversaries which may then form part of safety planning.
Acute care
During 2009-2019, over a quarter (29%) of patients died by suicide in acute care settings, including in-patients, post-discharge care and crisis resolution/home treatment. Of the estimated 67 suicides by mental health in-patients in 2019, half were on agreed leave. The highest number of post-discharge deaths occurred 3 days after discharge from psychiatric in-patient care.
We recommend clinical services address the ward environment (both physical and emotional), vigilance and the safety of leave arrangements before discharge. After hospital discharge, patients should be followed up within 72 hours of discharge. These recommendations are highlighted in our “10 ways to improve safety” toolkit.

People aged under 18
 During 2009-2019 there were 213 suicides by patients aged under 18, an average of 19 deaths per year. This represents 19% of general population suicides in this age group, a lower proportion than in older groups (27%). Recent numbers appear to be higher, reflecting the increase in general population suicides by people aged under 18.
During 2009-2019 there were 213 suicides by patients aged under 18, an average of 19 deaths per year. This represents 19% of general population suicides in this age group, a lower proportion than in older groups (27%). Recent numbers appear to be higher, reflecting the increase in general population suicides by people aged under 18.
We recommend that suicide prevention in young people should focus on access to services, with services ensuring they have the skills to address multiple co-existing difficulties, preventing and responding to self-harm, and specific diagnoses such as autism and eating disorders. We also suggest clinicians assessing risk consider enquiring about online experience.
Patients with recent economic adversity
 There were 281 deaths per year in patients who had experienced recent economic adversity, i.e. financial problems, workplace problems or homelessness. These patients were more likely to be middle-aged men, unemployed, divorced or separated, and were more likely to have recent illness onset, especially depression, and alcohol and drug misuse than other patients.
There were 281 deaths per year in patients who had experienced recent economic adversity, i.e. financial problems, workplace problems or homelessness. These patients were more likely to be middle-aged men, unemployed, divorced or separated, and were more likely to have recent illness onset, especially depression, and alcohol and drug misuse than other patients.
We suggest clinical services should be aware of the features of those at suicide risk in the context of economic adversity and should work with organisations that support people facing debt or other financial problems.
Patients with physical illness
Our findings show an increase in the number of patients with a comorbid physical illness since 2014, accounting for 25% of all patient suicides in 2009-2019 overall. The risk profile of these patients is not the same as for patients generally – they are older, common risk factors such as self-harm or alcohol/drug misuse are less often present, and a higher proportion are women.
We recommend clinical services should be aware of the risk from opioids prescribed for pain and we suggest clinicians assessing risk enquire about access to opioids available at home, particularly among older patients.
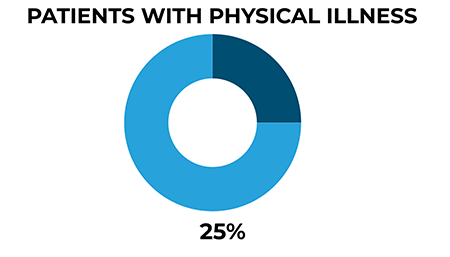
Patients with a history of domestic violence
 The majority of patients with a history of domestic violence were female. They were more often younger, single or divorced, living alone and unemployed than other women. Self-harm, previous alcohol or drug misuse and personality disorder diagnosis were more common in this group, potentially reflecting previous trauma or abuse.
The majority of patients with a history of domestic violence were female. They were more often younger, single or divorced, living alone and unemployed than other women. Self-harm, previous alcohol or drug misuse and personality disorder diagnosis were more common in this group, potentially reflecting previous trauma or abuse.
We ask clinical services to be aware of the risk associated with domestic violence, especially in female patients, but also in men. We suggest clinicians assessing suicide risk should include experience or threat of domestic violence.
Suicide prevention during COVID-19
 Findings from our real-time data collection of suspected suicide deaths in England during the pandemic show experiences such as anxiety, isolation, or disruption to care may have contributed to some suspected suicide deaths by mental health patients.
Findings from our real-time data collection of suspected suicide deaths in England during the pandemic show experiences such as anxiety, isolation, or disruption to care may have contributed to some suspected suicide deaths by mental health patients.
We suggest clinical services be aware of the need to maintain support for patients under the care of mental health services, particularly for patients who are anxious or isolated, or have experienced disruption to care.
